Research Article - (2022) Volume 6, Issue 3
Understanding who the public wants to communicate about radiation requires understanding how perceptions vary among different segments of the general population distinguished by varying degrees of familiarity with radiation topics. Radiation workers have a better understanding of Low-Dose Radiation (LDR) compared to the general population, but not a comprehensive one as demonstrated through survey and focus group results. Radiation workers that possess greater experience and understanding and who rank their knowledge about radiation as high are good candidate communicators but will need support. Scientists, followed by regulators, are the most trusted communicators, through peer reviewed articles and via education institutions. Radiation workers and the general public agree that more information about LDR is required and are concerned about the consequences of not improving the public’s understanding of LDR. The role of the regulator in educating both radiation workers and the general public was emphasized, and some very specific information programs were identified for the regulator.
Low-dose radiation, Public radiation knowledge, Communication, Population
Working with radiation, and exposure to radiation through medical testing and treatment have become increasingly important in the 21st Century with improved diagnostic procedures such as Positron Emission Tomography (PET) and Computed Tomography (CT) scans [1]. Nuclear methods are also important for solving diverse material science problems (for example, concerning improving electric vehicle batteries and determining structural weaknesses in structures). Several studies have documented that the North American population is increasingly exposed to Low-Dose Radiation (LDR), defined as below 100 millisieverts (mSv) of ionizing radiation [2]. The largest exposure is to naturally occurring radiation in our environment (37% radon and 13% other), followed by medical imaging (48%), airplane travel 2%, and nuclear power plants (~0%) [3]. the average person in the USA is exposed to between 0.5 to 3 mSv of LDR every year through CT scans and chest X-rays [4].
Studies confirm that the public has concerns and misperceptions surrounding sources and the risks of exposures to LDR [5-8], and there is a gap in people’s desires for more information and the provision of this information [6,9]. Public concerns include that all radiation exposures (including X-rays) are harmful (i.e., carcinogenic), that prolonged radiation exposures accumulate damage within our body, and children are more susceptible to radiation [10]. These mispercep- tions can have negative impacts including the refusal to accept medical treatments and interventions, including radiation therapy for cancer and diagnostic X-rays [8,11]. These concerns also exist in the field of power generation where nuclear energy is identified as an important future source of power production, but a gap exists in its implementation [12,13].
Science communication surrounding LDR and its risks are important in addressing misperceptions and concerns [14]. Medical professionals and people working with radiation and LDR are identified in the literature, based on their training, but also in the desires expressed by study participants, as key communicators to help address the public’s misperceptions and gap in knowledge [8,15,16]. This research addresses the questions:
1. Do people working with radiation have the knowledge and capacity to be LDR communicators?
2. What communication and knowledge dissemination should occur concerning LDR and radiation, and who should disseminate it?
Radiation Knowledge and Radiation Worker’s Communication Role
The ‘deficit model’ or idea that filling the public’s misunderstanding or lack of understanding of science with science, communicated by scientists [17], has been deeply criticized. This is largely due to its application in a unidirectional manner (from scientists to lay person) [18], and of course its initial failure to account for the behavioral science outlined, which has since been rectified [19,20]. In addition to substantive scientific knowledge and scientific methods, the impact of science on individuals and society is a key component in science education and communication [19,21].
So, addressing the confusion and misunderstanding surrounding LDR and its health risks with prolonged engagement to increase understanding of science and uncertainty has benefits [6,22]. This method helps make people less anxious and better at coping with risk and decreases their negative perceptions of nuclear issues [5,23]. However, this activity departs from the historic unidirectional science presentations to the public, into a multi and interdisciplinary activity. This radiation and LDR information dissemination activity includes fundamentals of education and psychology with considerations of affect, and trust [8,19,23].
The higher people’s trust in a communicator, the more stead is placed in the information they receive, and in respect of radiation, the greater they estimate benefits and the lower they estimate risk [8]. Thus credibility, or the ability and power to inspire belief in one’s statements [24], is a key determinant of the impact, of communication and veracity of information provided [25].
Medical professionals and people working with radiation and LDR are key communicators and are credible trusted sources of radiation information. They help address the public’s misperceptions and their gaps in knowledge [8,16,15]. However, studies have documented that people working with radiation and medical professionals also can have confusion and misunderstanding surrounding LDR and its health risks [6,22]. This medical/nuclear experts also think and express LDR and radiation risks differently from laypeople [5]. Physicians focus on medical benefits and risk in terms of medical results while physicists focus on radiation delivery and keeping doses as low as reasonably achievable. Epidemiologists express risk in terms of effects in a population [8]. So, while there is a clear basis in the literature for the importance of medical and radiation experts in communicating to the general population around radiation and LDR, there is cause for further investigation. Questions surround which medical professionals and people working with radiation should be communicating (based on understanding of LDR and radiation), what types of methods and framings should be used, and what methods of engagement are best?
This research reports the results of a mixed method study of a survey and qualitative research using focus groups. The survey was conducted by telephone in the provinces of Saskatchewan (western) and Ontario (central) Canada, the former being a uranium mining province and the latter a nuclear power dependent province. 1,104 respondents participated in Saskatchewan and 1,008 in Ontario during the months of November 2019 to July 2020. Respondents reflected the population in respect of gender and geography. In total, there were 1017 female respondents, 995 male respondents and 6 non-binary/third gender/other respondents. There were slightly more female than male respondents who took part from Saskatchewan compared to Ontario. In total, there were 151 Indigenous respondents and 1,863 non-Indigenous respondents. There were more Indigenous respondents from Saskatchewan (101) than from Ontario (50). While older respondents were the most numerous (65-75) followed by the middle aged (55-64); younger respondents were less well represented.
Respondents were asked if they have experience with radioactivity. Specifically, “Do you have personal experience working in a job that involves the use of radioactivity (e.g., in a nuclear power plant, in industry or in a hospital using radioactive sources, or from exposure to natural radioactivity in ores and other materials)?” Workers with such experiences are referred to as ‘radiation workers’. Approximately 22% of Saskatchewan respondents answered in the affirmative and 18% in Ontario.
At the end of the survey, participants were asked if they wished to participate in focus groups. Seventeen focus groups were conducted through 2020 and 2021 with a representative sample by gender and age. Thirteen of these focus groups were held with the general public, with six occurring in Saskatchewan and seven in Ontario. Four focus groups were held with radiation workers. There were two focus groups with radiation workers in Saskatchewan and two in Ontario. Two of the radiation workers focus groups (one from Saskatchewan and one from Ontario) had all participants who indicated a high level of self-ranked personal knowledge of radiation and possessed a higher level of knowledge on radiation based on their responses during the focus group discussions. The other two radiation workers focus groups contained a mix of participants with higher and lower levels of knowledge of radiation. This composition was not preplanned but was determined by analyzing the focus groups based on the participants rating their own knowledge and their ability to answer questions surrounding LDR and radiation topics correctly.
Participants were screened for age and gender representation. The first four focus groups in Saskatchewan were held face-to-face, but after March 2020, focus groups had to be conducted online using Zoom due to COVID 19 restrictions. Information about focus group participants appears in Table 1.
| City | Total | Radiation workers | Total | |
|---|---|---|---|---|
| Saskatchewan general public |
||||
| Estevan | 5 | #1 All experts | 8 | |
| Regina | 9 | |||
| Saskatoon | 11 | |||
| Swift current | 7 | #2 Mixed | 6 | |
| Saskatoon | 8 | |||
| Regina | 9 | |||
| Total Sask | 49 | 14 | 63 | |
| Ontario | ||||
| Toronto | 9 | #1 Mixed | 6 | |
| London | 9 | |||
| Ottawa | 8 | |||
| Hamilton | 8 | #2 All experts | 5 | |
| Thunder Bay | 7 | |||
| Sudbury | 7 | |||
| Owen Sound | 6 | |||
| Total Ontario | 52 | 11 | 63 | |
| Total | 101 | 25 | 126 | |
Table 1: The demographics of the focus group participant.
The focus groups were taped, and conversations were transcribed and then analyzed using both NVivo qualitative data analysis software and SPSS (Statistical package for the Social Sciences software). Coding was both thematic (utilizing the focus group guide) but also inductive whereby multiple variables that included new themes were created and then the focus group were compared to identify similarities and differences, as well as place-based themes.
This section analyzes and highlights significant differences between research results concerning the general population and people that identify themselves as radiation workers.
Understanding of Radiation and LDR
Radiation workers perceive their knowledge of radiation to be greater than that of the general population. Radiation workers were more likely to rate their personal knowledge about radiation as either ‘very good’ or ‘good’ than were respondents who did not have this work experience. Conversely, respondents not working in either a nuclear power plant or with radioactive sources were more likely to rate their personal knowledge as either moderate, poor or very poor, as depicted in Figure 1.
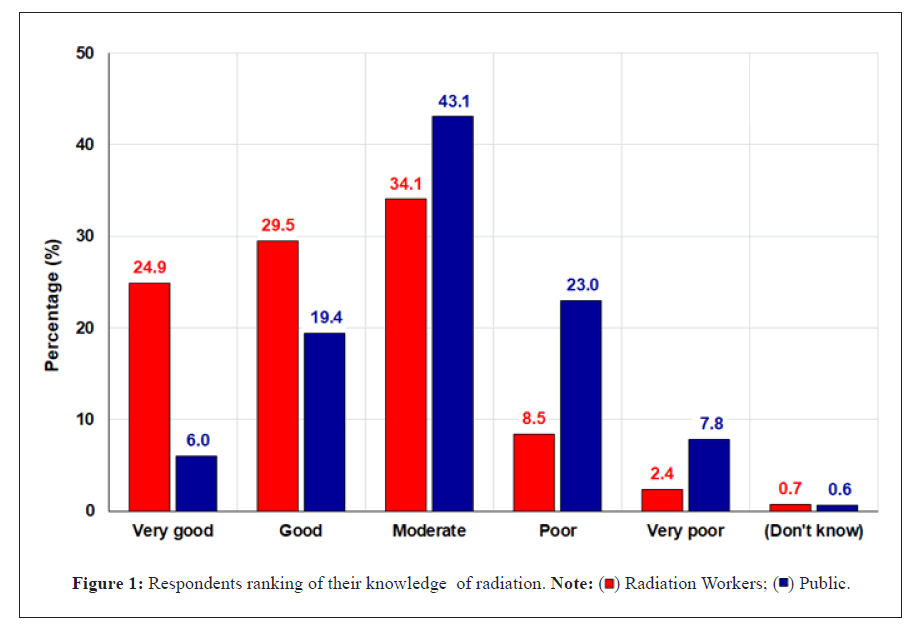
Figure 1: Respondents ranking of their knowledge of radiation. Note:  Public.
Public.
Consistent with previous literature assessing the understanding of LDR and radiation [6,2,22], both the survey and focus groups confirmed misperceptions and a deficit of knowledge. When asked if there were two types of radiation, ionizing and non-ionizing, the percentage of right answers was highest among radiation workers. Respondents working with radiation were more likely to answer this question correctly (65%) while fewer of the general population answered this question correctly (52%). However, a significant percentage (20%) of radiation workers either answered the question incorrectly or did not know the answer. Non-radiation workers had the highest percentage answering “Don’t know;” 14% more of the general public answered don’t know to this question, compared to radiation workers.
The degree of knowledge demonstrated by radiation workers versus that in the general population was less divergent in the survey than in focus groups. Stated another way, the radiation worker focus groups reflected participants with high levels of knowledge, while the general population focus groups reflected people with much less or no radiation knowledge. In the general population focus groups, only three participants admitted having heard about ionizing and non-ionizing radiation previously, and only one provided the correct definition of ionizing radiation. Radiation workers fared better. Most participants knew the difference between ionizing and non-ionizing radiation. Several were well versed and trained other employees in relation to radiation and safety. In the general public focus groups, very few knew what a half-life was, while most in the radiation workers focus groups did. These differences may be explained by the differing methodologies employed in surveys and focus groups. In the survey questions, the chances of answering true or false questions accurately are higher than answering a direct question about what is ionizing radiation in a focus group. Further, it is relatively easy to self-identify as a radiation worker in a survey but participating in a focus group might require a greater degree of self-identification and interest. This would presumably also have implications for radiation workers that would self-identify and be willing to be communicators; it is anticipated a form of participatory selection or censorship as a communicator would occur.
The point relating to the participatory selection that occurred with those participating in a radiation worker focus group is further substantiated by the topics discussed within the radiation worker focus groups versus the general population. With radiation workers, the topic of ionizing radiation came up even before it was initiated by the moderator. In the two radiation focus groups that contained participants who all indicated a higher level of knowledge on radiation, several participants asked if the topic being discussed concerned ionizing radiation. Very early the participants in these two focus groups identified harmful ionizing radiation and non-harmful non-ionizing radiation. The misconception that non-ionizing radiation is harmless was not addressed, although radiations such as microwave, infra-red and ultra-violet radiations are far from harmless. In one of these two groups, a radiation worker immediately pointed out LDR only related to ionizing radiation, but there were other types of radiation and cell phones emit low-level non-ionizing radiation. In the other of these two groups, a participant immediately responded when asked if they had heard of radiation, “I am assuming you mean ionizing radiation and not a more general meaning of the word?” Clearly, this participant was aware of the electromagnetic radiation spectrum which spans radio waves to gamma radiation.
Confusing of LDR Definitions
Amongst radiation workers there is confusion surrounding the definition of LDR. LDR is defined as below 100 mSv of ionizing radiation [2]. Ionizing radiation has enough quantum energy to eject an electron and has the potential to physically change DNA, while non-ionizing radiation does not have enough energy to ionize atoms or molecules [26]. One of the mixed knowledge radiation worker focus groups assumed LDR, as defined for the studies, related to all radiation; the other mixed focus group and the two more knowledgeable radiation workers groups participants identified the context of the study and assumed that, in this case, LDR related only to ionizing radiation.
In the mixed radiation workers Ontario group that was confused on this topic, one participant knew to ask, “Are we talking only about ionizing radiation or also electromagnetic radiation?” The group discussed all forms of radiation (non-ionizing and ionizing). Several participants in this group were able to identify sources of LDR (X-rays etc.) correctly. The sun (a source of ultra-violet radiation) became especially important in the discussion, as one person had developed skin cancer because of their fair skin and overexposure to sunlight out of doors. When the discussions started to cover where LDR was found the participants suggested uranium mines, everywhere on earth, rocks, flights, and sun.
The general public focus groups generally identified LDR as levels of radiation so low as to not be harmful. Only a few participants could correctly provide a definition and identify its measurement. Radiation workers were more specific with a proposed definition of LDR. Many suggested ‘below the regulatory limits’, or ‘radiation levels that are low enough to not cause damage or sickness.’ The consensus of answers was below the thresholds that are considered harmful; it was acknowledged that these were non harmful limits only if not exposed too frequently. Radiation workers pointed out exposure times were important surrounding danger, and there were different theories mentioned including hormesis. Workers often pointed out that it was something they thought about because of work and sometimes because of the location of their homes and the possibility of radon gas in their basements.
Confusion Surrounding Sources of LDR
When asked to identify medical treatments that were a source of ionizing radiation there was no significant difference between the responses of radiation workers and the general population. 75% of respondents identified dental X-rays and chest X-rays as sources of ionizing radiation, but only 66% correctly identified a CT scan and just fewer than 60% a mammogram. 55% incorrectly identified an MRI and 35% incorrectly identified an ultrasound as giving ionizing radiation exposures. Radiation workers only fared slightly better. This is consistent with the literature which has documented that often even physicians do not know about LDR (with as many as one-third of non-radiologist physicians not being able to distinguish imaging examinations for which ionizing radiation is used from those that do not) [6,1].
General population focus groups also produced this finding. A few people in the general population just could not believe cell phones and microwaves do not generate LDR. One focus group eventually resolved it with the following discussion: “how is a cell phone not a source of low dose radiation?” and the same person, “I work in the tech field, so I hear it from time to time when talking about wireless communications in particular (which is low dose non-ionizing radiation).” Because the focus group was developed to ask questions and explore concerns, but not provide information to fill an assumed deficit, confusion surrounding radiation, ionizing and non-ionizing, and the definition of LDR was not resolved.
A few radiation workers also experienced a similar confusion; however, most radiation workers in focus groups did correctly identify the medical treatment sources of ionizing radiation. From the radiation worker focus group discussions, the initial explanations of ionizing appeared to influence the group into deferring to the early identified knowledgeable participants for answers. This provides an explanation for why the radiation worker focus group discussions were more accurate than the radiation worker survey results. Radiation workers were more accurate in identifying where LDR occurs naturally in soils, rocks, airplanes (sky), potassium in your own body, radon in your basement, sources at work, helping crops survive, helping people with illnesses, and sterilizing [27].
In the general population focus groups, people in Saskatchewan identified radon gas as a source of radiation. One participant stated:
“From what I read, the radon gas is the source of background radiation that has the most impact on us, the most millisieverts. But I think its two millisieverts a year, if I read correctly. But the problem is when it becomes trapped or condensed, I think, in a space or in a work site. So, I think that’s why they’re selling radon kits and stuff now. I’ve seen more on that too.”
Radon was also identified in the radiation workers focus groups as a source of LDR but there was very little, if any, discussion about it.
Correlation of Confident Radiation Workers with Correct Answers
Because radiation workers were not significantly better at identifying medical treatment sources of ionizing radiation than the general population, and only 14% answered the question surrounding the two types of radiation (non-ionizing and ionizing) correctly, we analyzed the survey results to check for a correlation between survey respondents identifying their level of knowledge as high and answering questions about radiation correctly. Figure 2 shows that those radiation workers that identified their level of knowledge as either moderate, good, or very good to a greater extent than the public were much more likely to answer correctly ‘true’ to the question about whether there were two types of radiation (ionizing and non-ionizing).
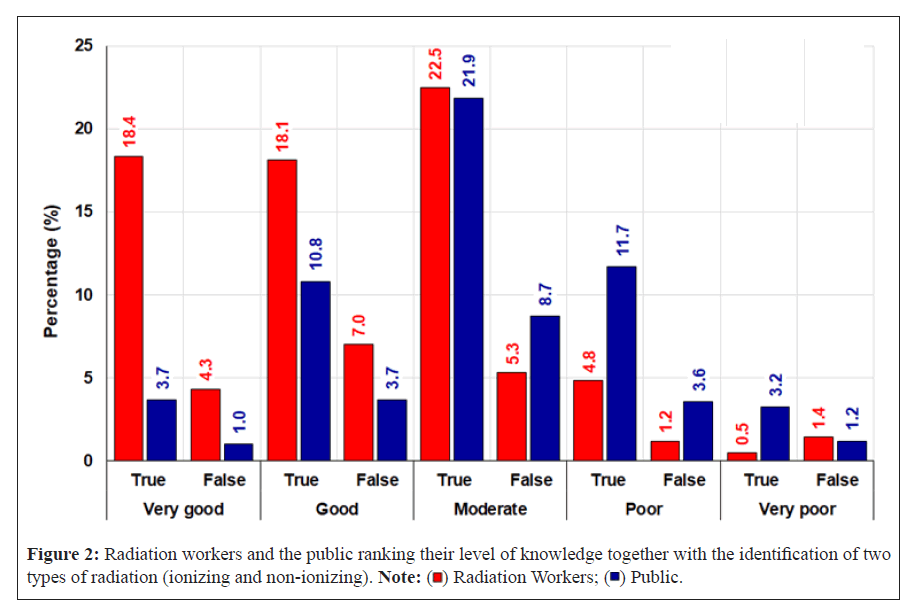
Figure 2: Radiation workers and the public ranking their level of knowledge together with the identification of two
types of radiation (ionizing and non-ionizing). Note:  .
.
However, when we considered the level of knowledge of radiation workers and the general public together with answering questions correctly about whether medical diagnosis of MRIs and ultrasounds involved ionizing radiation (the answer which is No) we obtained different results. Significant numbers of both the public and of radiation workers, regardless of level of knowledge, answered this question incorrectly. It was quite surprising to see radiation workers who identified as having either good or very good levels of knowledge faring poorly. Almost an equal number of those answering that MRI did not have ionizing radiation believed incorrectly that it did have ionizing radiation.
Radiation workers and the public fared better in identifying ultrasound as not a source of ionizing radiation. As depicted in Figure 3, a greater number of radiation workers who identified as having very good, good, or moderate knowledge answered the question correctly that an ultrasound does not have ionizing radiation. Similarly, a greater number of the public with poor, moderate, good or very good knowledge answered correctly. More research is required to understand why radiation workers that identify as having either poor or very poor knowledge about radiation answered this question incorrectly compared to the general public. Also, more research is needed to understand why both the public and radiation workers have a greater understanding surrounding ultrasounds and ionizing radiation than they do about MRIs. It could be differences in the frequency that survey respondents have undergone an ultrasound versus and MRI, but further substantiation of this would be required.
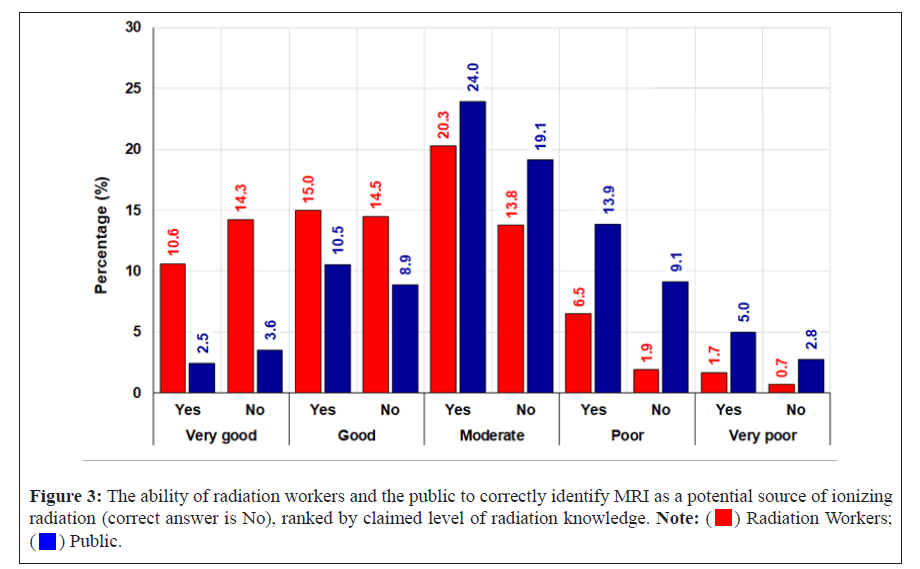
Figure 3: The ability of radiation workers and the public to correctly identify MRI as a potential source of ionizing
radiation (correct answer is No), ranked by claimed level of radiation knowledge. Note:  .
.
The results of the survey and focus groups showed that most radiation workers do correctly identify that there are two types of radiation (ionizing and non-ionizing), especially those with a moderate to very good knowledge, to a greater extent than the public. However, misunderstanding of LDR in relation to an MRI exists both within the radiation workers and the public in groups at all levels of declared knowledge. There is a better understanding of ultrasound. People who identify as radiation workers and self-select to participate in a focus group have higher levels of knowledge and could potentially be better LDR communicators. However, both survey respondents and focus group participants were asked questions about what people they preferred to receive information about radiation from, their associated levels of trust in these people and what information channels they preferred for receiving this information, which is covered below in section 4.3.
Who is Trusted to Communicate about LDR?
Credible and Trusted Sources of Information: Survey respondents ranked the people they preferred to receive information from about LDR in the following order: scientists (40%), the nuclear regulator (the Canadian Nuclear Safety Commission [28]) (25%), health professionals (18%), followed by environmental groups (5.4%), and industry (1.5%). The only significant difference between radiation workers and the public related to receiving information from the CNSC as 10% more radiation workers expressed a preference for receiving information from CNSC than did the general population (Figure 4).
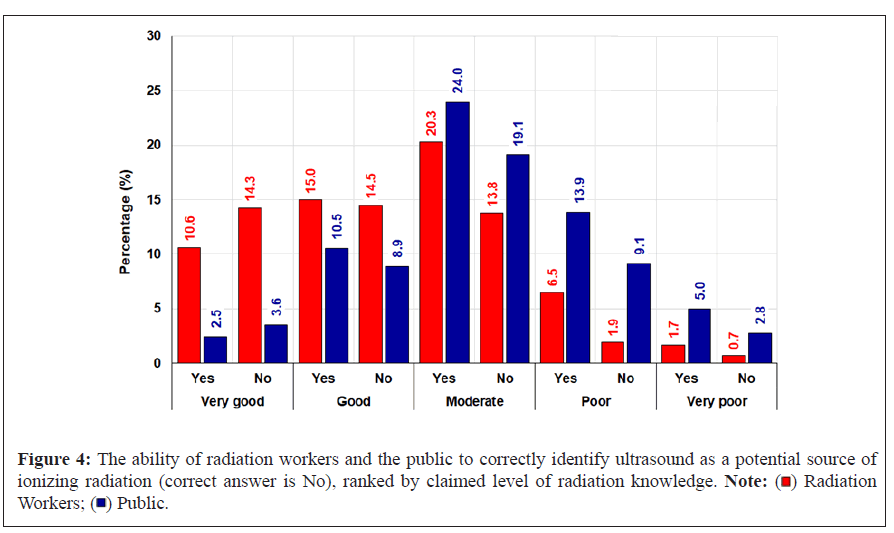
Figure 4: The ability of radiation workers and the public to correctly identify ultrasound as a potential source of
ionizing radiation (correct answer is No), ranked by claimed level of radiation knowledge. Note:  .
.
Those identified as a credible source of information were also identified as trusted to provide information, in the same order. Trust is an important component of whether expert information is judged as credible. Increasing trust in communicators has also shown to reduce peoples’ perceptions of risk and increase their estimated benefits [8]. When survey respondents were asked who they trust as a credible source of information when they hear about radiation, scientists were ranked number one, followed by the regulator Canadian Nuclear Safety Commission (CNSC), environmental groups, industry representatives, and elected officials, in that order. The most distrust was expressed for elected officials, followed by industry representatives, and then environmental groups.
In the focus groups there was a deeper nuanced discussion of trust. Although scientists were identified as the most trusted there were caveats identified. “If it is their field of expertise and there is a consensus among a majority of them.” But questions did arise surrounding who is sponsoring research and there were always a “few bad eggs” out there. Another stated, “Scientists would be trusted, if the scientist is not directly linked to a specific company.” Another stated, “I trust scientists too, but even they can be swayed by a pay cheque or political agenda.” Another added they trusted “the honest ones only.”
Radiation workers focus groups also identified a whole new group of experts. While there was general trust for scientists, participants drilled deeper and identified people with a Ph.D. in a nuclear topic, medical physicists, members of the International Commission on Radiological Protection (ICRP) and the United Nations Scientific Committee on the Effects of Atomic Radiation (UNSCEAR), the ‘green man’ (radiation protection employees at work), the health and safety department employees at work, and experts in Health Canada.
The general population trusted nuclear regulators, but radiation workers had even greater trust in nuclear regulators. People with experience working with radiation had significant higher responses (32.6%) that they ‘trust completely’ the CNSC than those without experience (23.6%). Radiation worker focus group participants spoke highly of the CNSC, often preferring the regulator over a scientific journal article. “The regulations have been established based on ‘YEARS’ of research.” One radiation worker stated, “The radiation officials I’ve come across are very well educated and experienced in the field, so I trust them. They aren’t ‘politicians’ or anything.”
Medical professionals were identified as trusted after scientists and the regulator. The family doctor was sometimes identified by the general population group, but preference was expressed for those working in cancer clinics, including radiologists and oncologists. Radiation workers were a bit more nuanced and immediately recognized that general practitioners may not be that knowledgeable. Health care professionals depended on their expertise and experience, and focus groups agreed that ‘health professional’ was a broad term. Generalists were identified as not very reliable. A few identified dentists. These sentiments are consistent with Evans et al.; a study which found only 39% of people had confidence that their health care worker was a reliable source of information.
Both focus groups and survey results show there is less trust in elected representatives of government, industry and companies, than in scientists, regulators and medical professionals. Radiation workers placed slightly more trust in industry in the survey than did the general population (with 6.3% stating they trusted industry completely while only 3.6% of the general population did). However, in the focus groups, radiation workers were split on the issues surrounding trust and industry and companies. Some were amenable to companies. One stated “in general OK but the public likely doesn’t think so,” another stated, “usually okay but can be self-serving,’ another “mixed-profit and pressure from shareholders can affect their point of view,’ and another ‘not reliable as they put their own interests ahead of the public unless they are heavily regulated like the nuclear industry.” These findings are similar to those of Dauer et al. Who also documents that people recognize bias in relation to its source. One general public participant thought that SaskPower was political and that politicians filtered their communications.
Radiation workers trusted environmental groups less than the public. 42% of radiation workers and 37% of the public chose ‘Do not trust at all’ or ‘Trust a little’ for environmental groups. This distrust was confirmed in radiation worker focus groups. Specifically identified were activist groups and non-government organizations. These groups were compared to the anti-vaccination movement as they “only stated opinion supported by falsehoods”.
How People Prefer to Receive Information?
More radiation workers identified education institutions as their main source of information about LDR than did the members of the public and fewer radiation workers identified the internet, TV, newspapers and CBC radio as their sources. Otherwise, by order of information source preference, survey respondents identified education institutions and the internet, TV, newspapers, friends and family, and magazines (Figure 5).
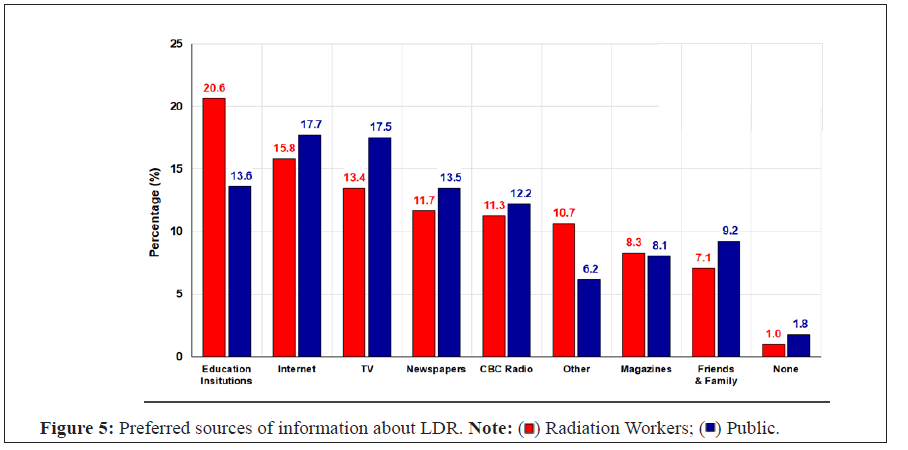
Figure 5: Preferred sources of information about LDR. Note:  .
.
Most focus group participants admitted to ‘Googling’ for information and using Wikipedia as their first ‘go to’ source to answer their questions. In the general focus groups, many stated their knowledge surrounding LDR came from family and friends that either worked in the nuclear industry or who had undergone medical/cancer treatments. This finding confirms that of Harris [15] which found that STEM professionals can play an important role in guiding the views of others on nuclear and radiation. In the radiation worker focus groups, participants confirmed that radiation was discussed at their workplace. For nurses, workplace discussions were prompted by taking a patient down to a test, getting an X-ray or CT scan, or having a posting on a door that someone had received a cancer treatment and there was a low dose of radiation.
Radiation workers in focus groups were unanimous in identifying the media as ‘unreliable,’ ‘usually poor,’ and generally not reliable. Some stated ‘mixed’ as their assessment of the influence of newspapers, and big established newspapers were regarded as more trustable. The New York Times was identified several times by radiation workers. A few stated the media had to be independent of religions and political parties. Specialist publications were also identified as ‘not bad’ and specific scientific or technical magazines, marketing research and engineering publications. Reference was also made to the CNSC regulations and the Canadian Guidelines for the Management of Naturally Occurring Radioactive Materials (NORM).
Both the general population and radiation workers identified social media as unreliable, and radiation workers used strong language. Words used included ‘completely unreliable’ and statements such as “I avoid social media like the plague.” Social media was described as a “complete cesspool of misinformation, propaganda, outright lies, and conspiracy theories,” and “like lemmings to the cliff.” However, no one in the general population focus groups could identify a time they received LDR or radiation information on social media. Only one radiation worker in the non-mixed groups identified information on social media about radiation, but it was posted by scientists working with radiation.
What should be Communicated by Whom?
Focus group participants were asked what specific information about LDR they thought should be provided to the public and who should provide this information.
What LDR Information should be Communicated?
The survey and focus group results document the need for more information surrounding radiation and LDR, the best people to provide this information, and which types of media are best for dissemination. Focus groups also provided an opportunity to delve deeper into specifically what types of information people were interested in and what strategies to use for dissemination.
The general public expressed a desire for more information on the sources and types of LDR, how it is measured, and the effects of LDR on humans (including on their genetics, and children (or procreation). The general public was very interested in understanding the benefits of LDR as well as the detriments and risks. Understanding how to prevent unnecessary exposure and methods to make nuclear power safer were also identified. One person stated, “I think its basic scientific knowledge, which is good to know, so people don’t fear ‘radiation’ like a bogeyman.”
Radiation workers did not express a desire to learn any more about the basics of radiation and LDR. Instead, they wanted to know more about who regulated what aspects, more about sources of LDR, more about LDR and electricity production, the effects of ionizing radiation on humans (such as in a university course). Some wanted to know about LDR in their specific community, daily lives, and ideas for prevention.
Radiation workers expressed a general liking for radiation and for learning about it. They were generally curious to learn more about LDR, even though their knowledge level was much higher than that of the general population participants. One acknowledged “I’m sort of weird.” Many of the general population focus group participants stated that they would spend some time after the focus groups to research and find out more about LDR. Focus group results confirm other studies that have discovered a desire for more information, and a deficit in providing it [6,9].
In the radiation workers focus groups, it was generally agreed that the general public was not knowledgeable about radiation. However, a discussion indicated that a chasm of ‘who believed the other was crazy’ exists. One radiation worker stated, “its crazy how un-educated the general public is.” Another radiation worker stated, “Everyone I speak with, when I tell them about my dreams to build thousands of nuclear power plants, think that I am completely crazy.”
The framing of information and risk communication was also thought to be a priority. Differing levels of knowledge, and different communication methods were identified as an important consideration within the focus groups. Within the two mixed radiation workers focus groups, the more knowledgeable participants pointed out that not all workers with radiation can be deep ‘experts.’ This was confirmed when their fellow participants were incorrectly answering some of the LDR technical questions. Future research will aim to understand the optimal interaction context, and the best way to advance learning about LDR and radiation in general. Within the groups of mixed radiation workers, and within the general population focus groups, the importance of acknowledging differing affects (emotions), levels of understanding and potential negativity bias were expressed by participants [29,30].
The more knowledgeable radiation workers framed risks and benefits very differently than those participants with lower levels of understanding, as determined by Perko [22] and Dauer et al. [8]. In focus groups, more knowledgeable radiation workers felt LDR, and nuclear power production was not a significant risk where others were more concerned. Future research to determine the impact of these radiation workers communicating this information, and information surrounding LDR, radiation, and nuclear power production on others is required. Of course, the manner, content, and duration of such communications, and the change in perceptions of recipients are future research questions as well. Previous research has identified medical professionals as key communicators surrounding LDR [8,16,15], but expanding these communicators into nuclear industry, mining, and nuclear science offers new possibilities.
Radiation workers placed the most importance on the goal of providing the public with more information to dispel common misconceptions, so “the public wouldn’t overreact to it, and to counter the anti-nuke hysteria and mis-information.” Radiation workers felt this was needed to put information in context, prevent hysteria, mistrust, negativity, fear, ensure people are properly educated and can make informed decisions whether to support the nuclear industry or not. In fact, radiation workers worried about how misunderstood LDR is; one stated, “Fear mongering was counter-productive, and without proper, easily understood information out there, many issues will happen.” Radiation workers identified the harmful effects of ‘fear:’
Because people fear what they do not understand, and if they don’t understand radiation, they will always fear it. There’s no ‘real’ reason to fear radiation.
Fear is a dangerous driver of change, and with anything, if the proper information is not out there and understood, we will have many issues; I believe the term used now is ‘sheeple.’
Specific things that need to be communicated to the public are identified in Table 2.
| Nuclear events | Fukushima Chernobyl |
An accurate understanding of the circumstances and consequences of these events |
|---|---|---|
| Basic information | The work being done to make sure the public stays safe. Pure information, objective data, with no hysteria or agendas. Simple, practical information so we can react and make decisions surrounding nuclear in our daily lives. “I like numbers; I hate reading things like X-rays cause cancer.” Radiation is everywhere and all around us; more than most people know; what types are, and where located. What types we need to take precautions about and the types of precautions. Basics of time, distancing, shielding. |
|
| Risks | Locate radiation risk in comparison with other risks from human activity. Balance the risks with the benefits. Impact of efforts to protect health: quick payoffs are sunblock, bike helmets, protective clothing. |
|
| Comparisons | Naturally occurring radiation levels to human generated radiation levels. Charts illustrating chance of cancer in one’s lifetime in relation to different types of exposures (smoking, etc.). Charts showing the doses of various things (banana, dental X-ray, Chernobyl etc.) |
|
| Benefits | Radiation is not always a negative word. The nuclear industry is the best way forward for low carbon energy production. That nuclear is misunderstood and there are important things nuclear science provides to us. Compare ionizing radiation to Advil. Advil isn’t bad; but 37 Advil are. |
Table 2: Identified components of information programs.
There was a clear divide between ‘reasons for concern’ in the general population focus groups and in the radiation workers focus groups. Statements of the general population demonstrated cultural concern for people living near nuclear plants (whom they believed were exposed to radiation), while radiation workers expressed a different form of egalitarian thinking. For radiation workers, nuclear power was a solution to the problem of climate change. Based on the data collected in this study, it wasn’t possible to conclude if other ‘group identities’ such as hierarchizes (who see the world in structured, centralized terms) who are generally agreeable to nuclear power [31] dominated in the focus groups. Radiation workers wanted people to understand the risks of radiation and LDR in the context of other risks and to make conclusions about the appropriate levels of concern; it was acknowledged that some time will be required for this. Generally, all focus group participants felt public information sessions would be ideal. There was some discussion about who has responsibility for this.
Who should Communicate to the Public?
Survey and focus group results highlight the reality that radiation workers may not always have the required knowledge to educate about LDR, even if they self-identify as having either good or very good knowledge. However, this group should not necessarily be discounted. As identified in 4.3.2 and by Harris [15], often STEM professionals are called upon by people for answers. Given self-selecting radiation worker focus group participants tended to be very knowledgeable, self-selection for dissemination activities might be preferable. Further, buttressing this group’s information and dissemination skills would be warranted in the light of the findings. Others were also identified. The identification of scientists (discussed in previous sections) is also germane to this section and focus group participants pointed out that scientists had a responsibility to disseminate information that was beyond the normal requirements of their role as university, government, or industry scientists.
No one group of communicators was identified by participants; several were. The importance of trust was emphasized with scientists and the nuclear regulator most often identified. Radiation workers identified people within their organizations who were experts. Medical professions were occasionally identified; however, the limitations of health professionals were also identified. The limitations of medical professionals without radiation training and experience were noted. Consistent with Kim [5] and Kahan [23] a multi-disciplinary and extended interaction with people was preferred. The general population focus groups and the radiation workers focus groups considered issues of affect, psychology, and trust as key concerns (as has previously been identified in the literature [8,19,23].
Radiation workers believed the nuclear industry and government need to better educate the public on the true nature of nuclear technologies. One stated accurate information is a human right and knowledge is empowering. Another participant pointed out “the government has been trying for years to do that but there is an incredible amount of misinformation that is like loud static.” Another participant (a nuclear safety educator) stated, “It is difficult to try and make them all experts on radiation. It might be hard to educate people and change people’s mind with one quick class.” Band-Aid solutions are not the answer, but focused concerted attention is needed.
There were sentiments that responsibility also rested with people and businesses. One radiation worker focus group thought Canada had proper rules and regulations but identified a responsibility of citizens to obey rules (for example, in relation to exposures to the sun, and the use of sunblock, and hats). Several radiation workers focus group participants expressed the view that builders should also have an obligation to test and advise about radon in their buildings; the responsibility to obtain information should not rest solely with homeowners. So, even while government and industry were not ranked highly as credible sources, and were not ranked as highly trusted, they had a responsibility for LDR information dissemination. Creative ways of supporting the trusted scientists by government and businesses are in order.
The role of the regulator was identified by radiation workers in respect of educating radiation workers, but also the public. Some very specific information programs were identified for the regulator. These included:
• What are the sources of LDR?
• What levels of LDR are allowed?
• How are the levels of LDR regulated?
• How are the doses of LDR calculated?
• Is LDR very dangerous?
• When does LDR become dangerous?
• What is the nature of the regulator’s studies?
• To whom does the regulator turn to for information?
Radiation workers do have a better knowledge about LDR than the general public, but they are not infallible as many misidentified MRIs and ultrasound as involving ionizing radiation. Radiation workers will need concerted training and skill development, combined with self-selection to fulfill the role of LDR communicators. Survey and focus groups conducted in 2019-2020 confirmed there is a deficit of knowledge and misperceptions surrounding LDR and radiation. Radiation workers do have a statistically significant higher degree of understanding surrounding the two types of radiation (ionizing and non-ionizing), and less misunderstanding. However, radiation workers still answer questions inaccurately in relation to sources of LDR. These findings from Ontario and Saskatchewan, Canada, are consistent with similar findings at other locations.
Among total survey respondents, preferred people to receive information from about LDR who coincided with the most trusted communicators included: scientists (40%), the nuclear regulator (the Canadian Nuclear Safety Commission (CNSC)) (25%), health professionals (18%), followed by environmental groups (5.4%), and industry (1.5%). Radiation workers had a greater preference and trust in CNSC and less trust in environmental groups and many information sources such as the TV, internet, and radio.
Research participants felt addressing misperceptions is important for the future of nuclear science, nuclear medicine, and the acceptance of its applications. Addressing the information deficit and people’s misunderstandings were identified as very important by focus group participants, and for science communication in particular.
Those who have different levels of experience and knowledge have differences in what they are interested in learning about radiation and have differing preferences as to how information is communicated in relation to risk. In this study both the general public and radiation workers had an interest in basic information about radiation and LDR and were passionate that learning more was important. However, the importance and desire for this was strongest among radiation workers. Top of the list for radiation workers was countering misperceptions around Fukushima and Chernobyl (and the movie with respect to the latter), basic information, risks (especially in comparison with other risks), and benefits. Very few participants in the general population focus groups knew of the benefits of radiation but wanted to know more. Understanding the benefits of nuclear science, but also of radiation, was an important component of public education identified by radiation workers.
More research is needed on how to frame information and risk communication and in what context it is provided. Different types of experts frame risk and its discussion differently and may not individually provide the correct solution in the correct context. For example, people with cancer experience risk in relation to medical treatment differently perceiving the benefits as important during their treatment. However, when cancer patients move to survivorship, their questions and perceptions of risk surrounding LDR change. Understanding how to communicate science surrounding radiation and LDR to different people, groups, and in different contexts will be an important research task, acknowledging people’s heuristics, affects and potential negativity bias.
Radiation workers trusted the regulator to communicate radiation information, and additional actors including workplace experts, to a greater extent than did the public. Radiation workers did not trust environmental groups as much. Radiation workers had a significantly greater interest in hearing about LDR from the regulatory body and education institutions than did the general population, but also preferred scientists. Health professionals also received support (but the deficits associated with certain health professionals were acknowledged. Radiation workers were also significantly less trusting of TV as a source of information and in focus groups were far more negative than the general population when assessing the possible role for social media in the communication of radiation information.
The work described was undertaken as part of the independent, low-dose research program “Addressing Public Concerns about Their Exposure to Low Doses of Anthropogenic Radiation” funded by the CANDU Owners Group Inc and by the Sylvia Fedoruk Canadian Centre for Nuclear Innovation.
This research was reviewed and approved by the University of Saskatchewan Behavioral Research Ethics Board (Beh-REB) that is constituted and operates in accordance with the current version of the Tri-Council Policy Statement: Ethical Conduct for Research Involving Humans (TCPS 2 2014). The University of Saskatchewan Behavioral Research Ethics Board reviewed this project and the proposal was found to be acceptable on ethical grounds, approval ID (Beh- REB) 1452.
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
Received Date: Oct 09, 2022 / Manuscript No: JNEPGT-22-76799 / Editor Assigned: Oct 12, 2022 PreQC No: JNEPGT-22-76799(PQ) / Reviewed Date: Oct 26, 2022 / QC No: JNEPGT-22-76799 / Revised Date: Nov 04, 2022 Revised Manuscript No: JNEPGT-22-76799(R) / Published Date: Nov 11, 2022 Doi: 10.11131/JNEPGT-22/1000012
Copyright: © 2022 H Margot, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.